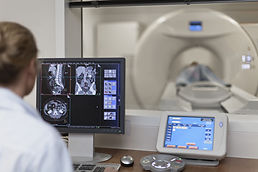

INformation
What To Do
Parents of children with brain tumours advise other parents to rely on their own "gut feelings". When you feel that your child is not what he used to be, do take the child to the doctor. Persistency of symptoms is also important. While it is appropriate to wait to take your child to the doctor if you observe the listed symptoms, if those symptoms persist, go to the doctor. If necessary, insist on the tests listed below, even if the doctor disagrees. On occasion, a child's teacher may notice a change in behaviour pattern or performance; take your child's teacher seriously. Ophthalmologists are sometimes the specialists who correctly diagnose brain tumours, so an eye exam is appropriate when vision problems are apparent.
Take your child to the doctor. The doctor should listen carefully to your description of your child's behaviour and ask you pertinent questions. If symptoms warrant, vision and other tests should be performed. The tumour probably will not be felt. The doctor should order tests:

Both of these tests are expensive, and therefore doctors will likely not order them until they rule out all other possibilities.
-
MRI
-
CT scan
As a parent, you may need to be quite insistent that they be performed. Any brain tumour will show up on an MRI; the CT scan misses some tumours.
Types of tumour
The following is intended to be only a brief summary of the information presented from other sites.
Most brain tumours are named for both type of cell from which the tumour originated and the location of the tumour in the brain. Often the common name of a brain tumour reflects the cell type from which it arose: "Astrocytoma" indicates that the tumour originated in astrocytes, star shaped cells that form part of the supportive tissue of the brain. More information about the tumour is included if you are told the name "cerebellar astrocytoma", indicating that it is located in the cerebellum in the brain.
Sometimes a general name is included in the name of a brain tumour, as in "brain stem glioma". Thus, the tumour is a glioma which is located in the brain stem. This name does not give any information about the type of glioma cell from which it arose. Glioma is a general term for tumours that arise from glial tissues, which are the supportive tissues of the brain. (Adenomas, usually benign, arise from a gland. Blastomas are malignant tumours whose cells have undeveloped or embryonic characteristics. A carcinoma is a malignant tumour that arises from skin or the lining of digestive, respiratory, or urogenital systems. Sarcomas are malignant tumours that arise from connective tissue, blood vessels, or the lymph system.) Brain tumours are usually either gliomas or blastomas. Often "glioma" or "blastoma" is included in the name of the tumour.
Certain types of brain tumours are more likely to occur in children because paediatric brain tumours usually arise from "young" cells, also known as immature or primitive cells. Common paediatric brain tumours are medulloblastoma, ependymoma, astrocytoma, brain stem and optical nerve gliomas, and gangliogliomas. However, any type of brain tumour can occur in children as well as adults.
MEDULLOBLASTOMA
Medulloblastomas arise from primitive neuro ectodermal tissue, or PNET. (PNET is a general term for a collection of many different brain tumours which arise from undeveloped brain cells.) Medulloblastomas are usually located in the cerebellum and are fast growing and highly malignant. They frequently spread, invading other parts of the central nervous system via the spinal fluid. Medulloblastomas account for the largest percentage of paediatric brain cancers. It is more common in boys than girls; it usually occurs between the ages of 2 and 6 (only 30% of medulloblastomas occur in adults); frequently spreads.
EPENDYMOMA
Ependymomas arise from the cells that line the internal surfaces of the brain, thus, they are gliomas. The tumours arise from "ependyma", cells that line the fluid spaces of the brain and spinal cord. Ependymomas located in the cerebral hemispheres occur primarily in children and adolescents. Although these tumours are capable of malignant behaviour, they are almost always benign.
ASTROCYTOMA
Astrocytomas arise from brain cells which form part of the supportive system of the brain, in particular, cells called "astrocytes" for their star shaped appearance. This tumour are usually slow growing and many are considered "curable". Astrocytomas are often cystic, in which case they are particularly easy to remove completely.
http://www.cancerbacup.org.uk/info/astrocytoma.htm
OPTICAL NERVE GLIOMA
These are slow growing tumours which form along the optic nerves. They usually occur children under the age of 10. The common cell type is pilocytic astrocytoma.
BRAIN STEM GLIOMA
These tumours, located in the brain stem, can be either slow or fast growing. Depending on the type of supporting tissue from which they arise, they can be either astrocytomas, anaplastic astrocytomas, glioblastoma multiforme, or a mixed tumour. In general, brain stem tumours are more common in children than they are in adults. Surgery is usually not possible in these tumours, and radiation and chemotherapy must be used instead.
OLIGODENDROGLIOMA
Slow growing tumours which arise from cells which make the myelin that insulates nerve fibres. They are located in the hemispheres of the brain, especially the frontal and temporal lobes, and in children are more common in the thalamus.
GANGLIOGLIOMAS
Usually slow growing, rarely malignant. These tumours can be located anywhere in brain, but are most often found in the temporal lobe. They arise from ganglia (a ganglion is a group of nerve cells). They occur most frequently in children and young adults.
CRANIOPHARYNGIOMA
Benign, congenital tumours. They are usually cystic and found primarily in children and adolescents.
MENINGIOMA
MIXED GLIOMAS
http://www.cancerbacup.org.uk/info/mixedglioma.htm
PINEAL REGION TUMOURS
The pineal gland is located in the posterior portion of the third ventricle. The most common tumour of the pineal region is the germinoma. Germinomas (germ cell tumours) represent over one-third of the tumours in this region. Germinomas of the pineal region are most common in teen-agers. Additional tumours found in this area include other embryonal type tumours, teratomas, astrocytomas, pineocytomas, and pineoblastomas.
ACOUSTIC NEUROMA
HAEMANGIOBLASTOMA
It has been brought to our attention that a "Leslie Christie" "Morrie Gunst" and other Aliases, has been informing people that we were shut down due to fraud??
This man is a sick and depraved coward that hides behind aliases to destroy the good work of the charity and its volunteers.
This charity has passed 26 years of audits and none of the office bearers or volunteers have benefited financially from the charity. In fact they have lost wages and time from their own jobs and lives to do the volunteer work.
It comes about from something that is unrelated to the charity.
He bitterly continues to abuse anyone that gave evidence of his abuse of his mother and other family members
A five-year Misconduct Restraining Order was awarded against him when he was abusive online to one of the volunteers of this charity, but he is now after 12 years of abuse targeting other family members in untruthful ways to indirectly be a nuisance (to say the least) to the volunteer. It would seem he has no conscience or care about the lives of others that only want to help people in need, or are in need themselves.
Please pray for his healing and hopefully he has an epiphany one day soon.